Quick Summary
We compared 7 credentialing platforms through the lens of what telemedicine organizations actually need: multi-state licensing, interstate compact support, continuous compliance monitoring, and the ability to scale PSV across a distributed provider workforce.
Here are the top 2 choices:
Looking for the Best Credentialing Solution for Telemedicine?
Credentialing a telehealth provider looks straightforward until you actually do it.
You:
- Verify their licenses.
- Check their board certifications.
- Pull their NPDB report.
- Confirm their DEA registration.
On paper, it looks like the same process as any other provider. But telehealth adds a layer of complexity that traditional credentialing workflows were never really built for. A physician practicing across 20 states means 20 licenses to track, different renewal timelines, and different state requirements to manage. That alone creates a lot more room for delays and mistakes.
This is not a hypothetical. One credentialing specialist managing a growing telehealth organization told us it takes her four to five hours to process a single provider file manually, going link by link through primary sources, pulling licenses, verifying board certifications, logging into CAQH separately from her credentialing system. That's before she touches the next provider in the queue.
Most credentialing software was built for hospital systems and traditional group practices. It handles the basics, but it wasn’t designed for the scale and complexity that multi-state telehealth organizations deal with every day.
If that’s the situation you’re in, the tools in this list are worth a closer look.
But first…
Why Listen to Us
Assured is an NCQA-certified credentialing organization that helps providers get credentialed in under 48 hours. While building Assured, we have spent a lot of time looking closely at other credentialing tools, too. Partly because you should know the market you are in, and partly because we hear the same pain points repeatedly in buyer conversations.
That gives us a pretty clear view of which tools make sense for different situations, which ones do not, and where our own platform fits in, too.
Why Telemedicine Credentialing Software Matters?
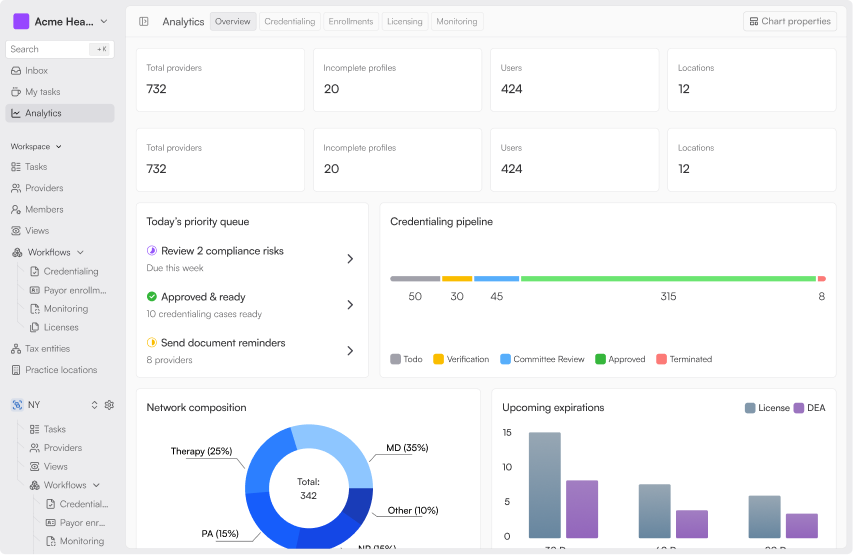
An uncredentialed provider cannot see patients or bill payers. Every day a provider sits stuck in a credentialing backlog is revenue left on the table. According to Bryson Tombridge from Tono Health,
“Not being able to get our doctors credentialed probably cost us $1M to $1.5M in the first year.”
For telehealth organizations onboarding providers at scale across multiple states, those delays add up fast.
Beyond revenue, there is also the compliance side of it. Credentialing is not something you do once and forget. Providers need to be recredentialed every two to three years, and their credentials need ongoing monitoring in between. Licenses expire. DEA registrations lapse. OIG exclusions can show up. If no one catches those changes, the organization can run into serious compliance and regulatory issues. And once you are tracking providers across 20 or 30 states, doing that manually stops being realistic.
The right tool does not remove the complexity, but it makes it much easier to stay on top of it.
The 7 Best Credentialing Solutions for Telemedicine Providers
1. Assured
Best for: Growth stage orgs and enterprises scaling credentialing and multi-state licensing
Assured is a credentialing software platform built for telehealth and other multi-state healthcare groups. We handle the full credentialing lifecycle, from primary source verification to ongoing monitoring, using AI-driven automation and a fully in-house credentialing team.
What makes Assured stand out is speed at scale. The platform automates verification across more than 2,000 sources, reducing the manual work that usually slows credentialing. We also integrate directly with CAQH, so we can auto-populate provider data without re-entering everything manually.
Assured returns credentialing packets within a 48-hour SLA, and customers often see first pass approval rates of up to 95 percent. For telehealth companies onboarding providers across multiple states, that difference shows up quickly in provider start dates and revenue.
For example, Blossom Health, a virtual psychiatry provider, used Assured to move from payer enrollment to roughly 72 hour submission timelines while scaling its provider network.

After the PSV is done, we continue monitoring credentials across thousands of sources, flagging expiring licenses, exclusions, and other compliance changes that become difficult to track manually at scale.
Key Features
- Automated primary source verification: Verifies provider credentials across 2,000+ sources without manual searching, cutting hours off each file.
- Direct CAQH integration: Pulls provider data straight from CAQH so your team isn't re-entering information that already exists.
- 48-hour credentialing SLA: Completed, audit-ready files back in 48 hours, at 100% compliance.
- Continuous monitoring: Tracks licenses, exclusions, and compliance changes after initial credentialing so nothing slips through.
- Expirables alerts: Flags upcoming expirations at 30, 60, and 90 days across your full roster.
- Flexible delivery: Full CBO, software-only, or hybrid, depending on how your team operates.
- Delegated credentialing: Achieve and maintain delegated status with Assured's NCQA-certified platform, ensuring you're always audit-ready
- Centralized roster management: Keeps your entire provider roster in one place with real-time status tracking across credentialing, enrollment, and compliance, so nothing gets lost in spreadsheets.
- All-in-one solution for credentialing, enrollment, and licensing: Handles credentialing, payer enrollment, and licensing workflows in a single system, removing tool-switching and giving your team full visibility end to end.
Pricing
Usage-based pricing that scales with provider volume.
Pros
- 48-hour credentialing turnaround with parallel PSV across 2,000+ sources, purpose-built for multi-state telehealth scale
- Sub-24-hour support with dedicated subject matter experts for telehealth
- All operations staff are direct employees, not third-party BPOs
Cons
- Newer company compared to legacy vendors
2. Symplr Provider
Best for: Health systems and academic medical centers running telehealth programs that need credentialing embedded within a broader governance, risk, and compliance suite
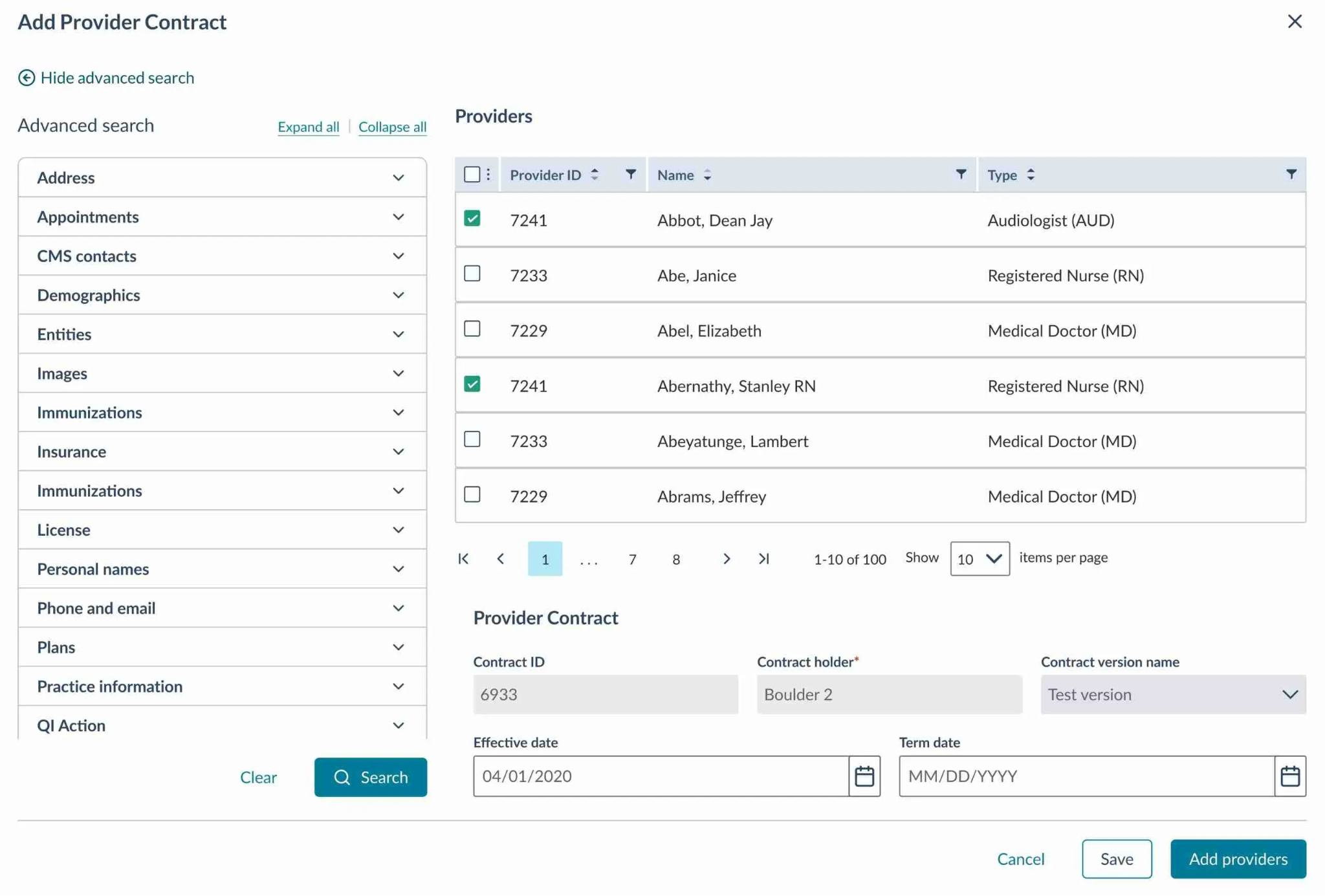
Symplr is a large enterprise healthcare operations platform that includes provider credentialing as one module within a broader suite covering workforce management, compliance, and contract management. It's built for and sold primarily into hospital systems and large integrated health networks.
The credentialing module handles primary source verification, provider file management, privileging workflows, and ongoing expirables tracking. For organizations that already operate within Symplr's broader ecosystem, credentialing as an add-on makes sense. The data flows between modules without additional integration work.
Key Features
- Centralized provider data management: Stores credentialing and privileging data across large, multi-facility organizations in a single location.
- Primary source verification automation: Connects to licensing boards, DEA, and national databases to verify credentials without manual outreach.
- Privileging workflow management: Routes clinical privilege requests and approvals through defined committee structures, designed primarily for hospital settings.
- Ongoing credential monitoring: Tracks expiration dates and compliance status across large provider rosters with automated alerts.
Pricing
Custom pricing based on organization size and modules selected.
Pros
- Broad GRC suite in the credentialing category
- Established track record across hospital systems running telehealth
- Multi-function platform extending beyond credentialing
Cons
- Users report slow performance and inconsistent support quality
- Capterra users flag gaps in forms management and data verification
- Complex implementation timeline
3. MD Staff
Best for: Hospitals and health systems managing telehealth as part of a broader credentialing and privileging operation
MD Staff has been in the credentialing software space for over 40 years and is used by more than 3,000 healthcare facilities. It has been ranked the #1 credentialing software by KLAS seven consecutive years running (2020–2026).
The platform is cloud-based and modular, with AI automation handled through its Aiva Credentialing engine for primary source verification against NPDB, licensing boards, and other regulatory databases. Its privileging, committee workflows, and performance evaluation makes it a strong fit for established health systems.
Key Features
- Aiva Credentialing engine: AI-powered PSV automation with automatic file flagging
- Modular architecture: Start with core modules and expand as your organization scales
- MD-Stat: OPPE and FPPE reporting tied directly to credentialing decisions
- State licensing board integration: Multi-state license verification synced to regional requirements
- E-Priv: Real-time, read-only provider privilege access for department staff
- Managed Care and Enrollment module: Payer enrollment handled within the same platform
Pricing
Quote-based monthly subscription. Varies by organization size, modules, and implementation scope.
Pros
- Ranked #1 by KLAS for seven consecutive years (2020–2026)
- 3,000+ facilities across 40+ years of credentialing-specific development
- Scales from small community hospitals to large multi-entity health systems
- Strong privileging and committee governance depth
Cons
- Built for hospital operations. Not designed around telehealth-first workflows
- No managed services; your team owns execution
- Implementation and customization cost extra on top of subscription
4. CredentialStream
Best for: Hospitals and health systems that credential telehealth providers by proxy and need deep privileging workflows with EHR integration
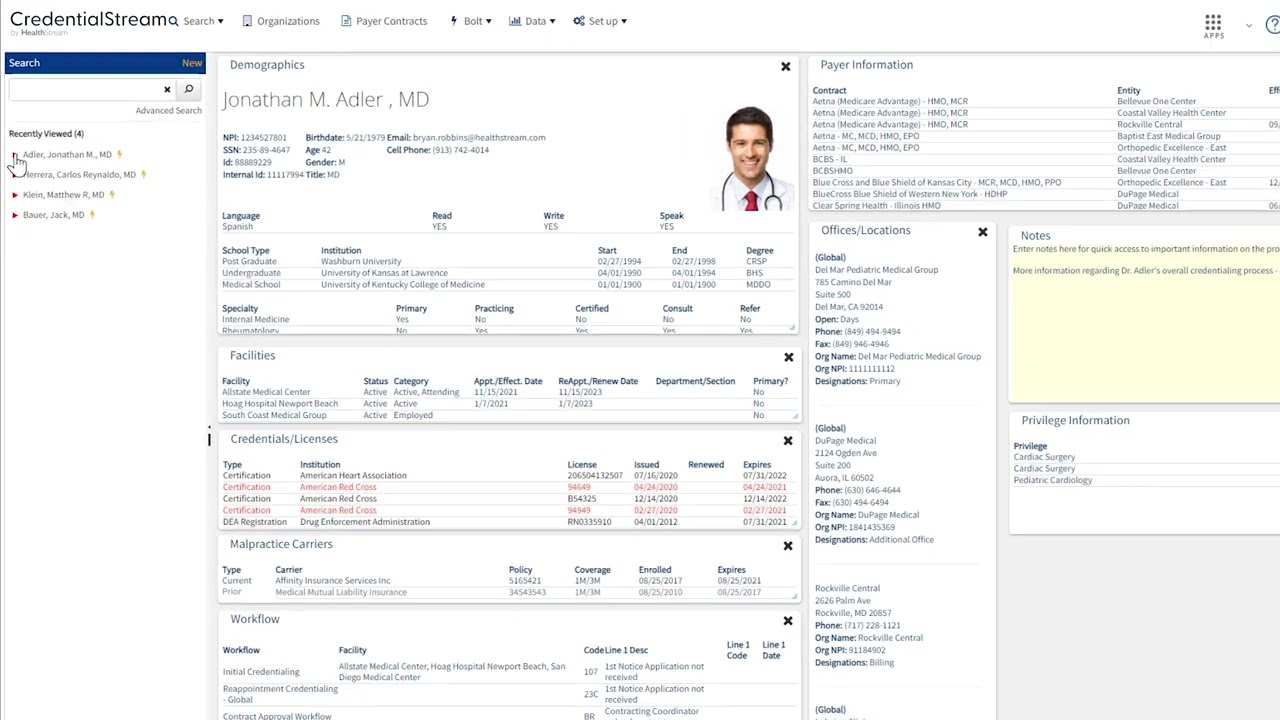
CredentialStream, now part of Verisys, is a credentialing and privileging platform built for hospitals and health systems. It automates the credentialing workflow, manages provider files, and integrates with primary data sources for verification.
Privileging is a core part of the product, which makes it well-suited for organizations where clinical privilege management is a central need.
Key Features
- Committee management: Route applications through structured review with configurable approval workflows
- OPPE/FPPE integration: Link provider performance data to credentialing decisions for evidence-based privileging
- EHR connectivity: Integrate with Epic, Cerner, and Meditech through the hStream platform
- HITRUST r2 certified: Meet the highest standard of healthcare data security and compliance assurance
Pricing
Subscription-based. Custom quotes based on organization size and modules.
Pros
- Deepest privileging capabilities available, including credentialing by proxy for telehealth
- Enterprise-grade audit trails and compliance reporting
- Direct EHR integration with major hospital systems
Cons
- Steep learning curve; users note complex report building
- Priced for enterprise budgets
- Not designed for growth-stage virtual care companies or smaller practices
5. Andros
Best for: Health plans and governmental entities building or expanding telehealth provider networks that need credentialing alongside a network strategy
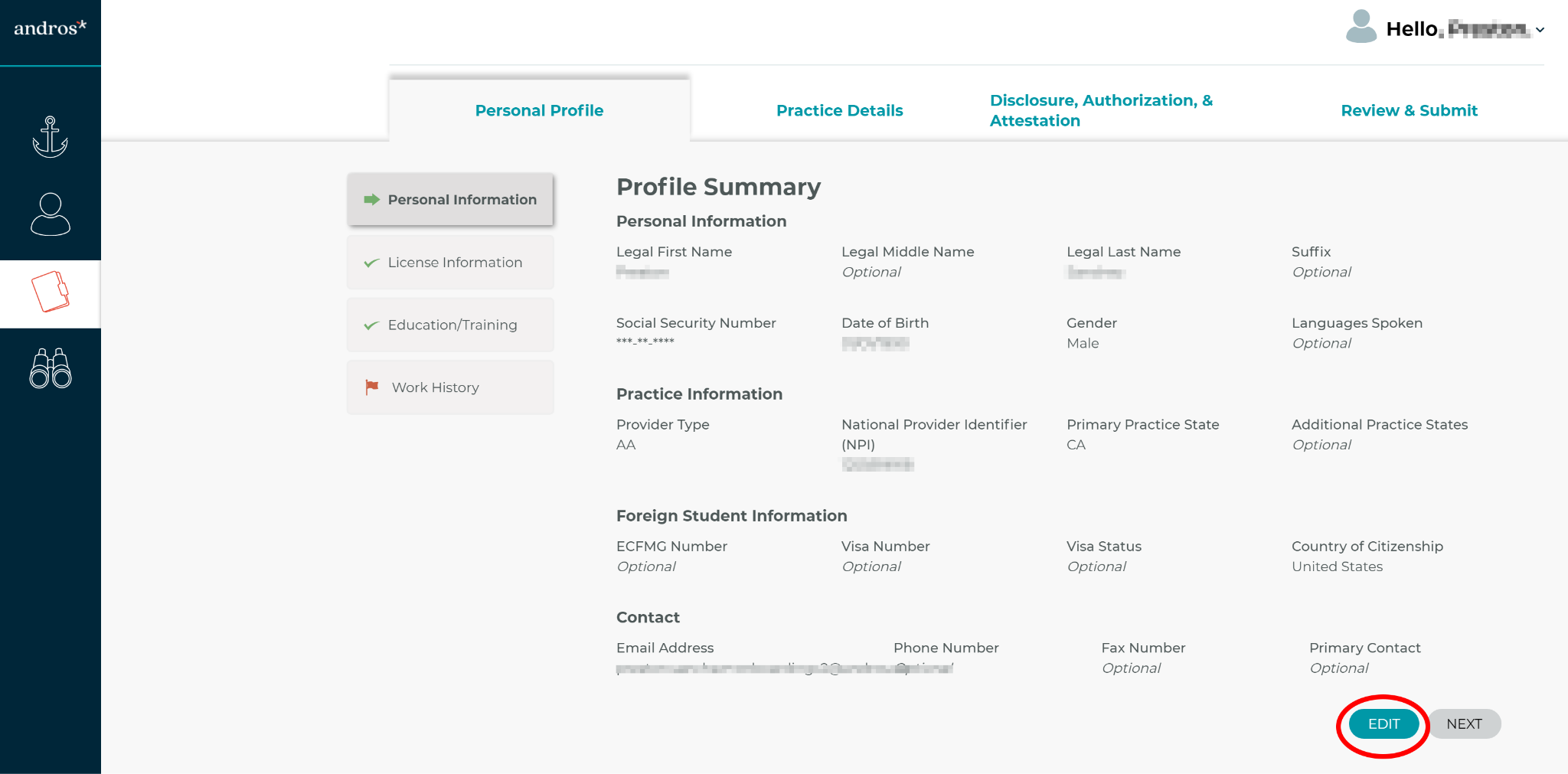
Andros is a provider data management and credentialing automation platform designed for health plans, large provider organizations, and networks that need to manage provider data at scale. Its focus is on the data layer: ingesting, verifying, and continuously maintaining accurate provider information across a network.
Andros operates more as infrastructure than as a credentialing workflow tool, so it tends to fit organizations that have credentialing processes already defined and need a reliable data foundation underneath them.
Key Features
- Data-matching PSV: Run instant verification with automated gap identification from a large verified provider repository
- Intelligent autofill: Complete most applications without requiring direct provider input
- Network lifecycle services: Cover strategic network design, provider recruitment, and payer contracting
- Committee management: Facilitate provider leveling, risk identification, and meeting coordination
Pricing
Custom pricing based on network size and service scope.
Pros
- Uniquely combines network strategy, recruitment, and credentialing in one platform
- Dual NCQA and URAC CVO certification
- Strong fit for organizations building telehealth networks from scratch
Cons
- Primarily oriented toward health plans and large network operators
- Full network lifecycle scope may be more than organizations needing credentialing only
- Platform login still runs on the legacy CredSimple domain
6. MedTrainer
Best for: Telehealth organizations that need credentialing and healthcare compliance training managed from one platform
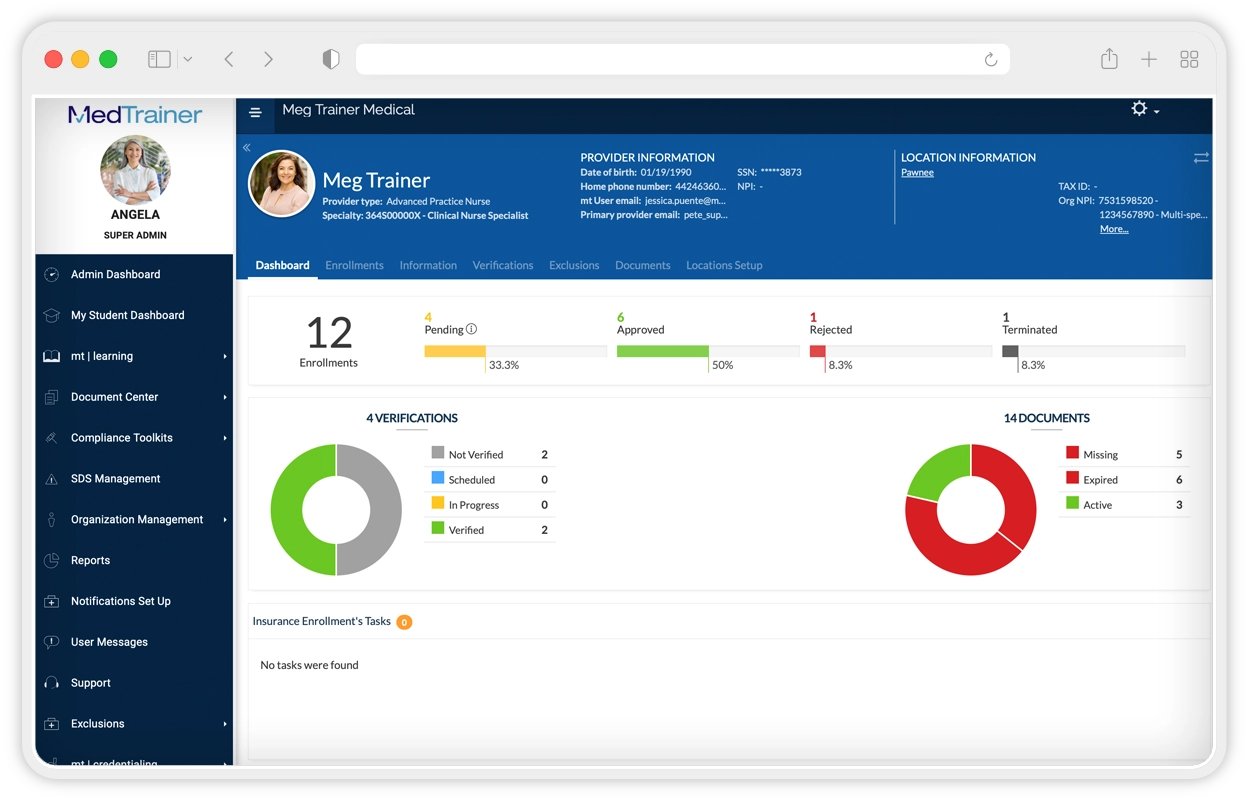
MedTrainer is a healthcare compliance and learning platform that also includes credentialing. It is mostly built for smaller practices, clinics, and ambulatory care teams that want to manage credentialing, training, and compliance in one place.
Its credentialing module covers the basics like provider file management, primary source verification, and expiration tracking. The setup is fairly approachable, which can make it a practical option for teams that do not have dedicated credentialing staff. For telehealth organizations with a smaller provider count and lighter credentialing volume, that all-in-one setup can be a real plus.
Key Features
- Three unified modules: Manage credentialing, compliance, and healthcare-specific LMS
- Exclusion monitoring: Run automated screenings across several federal and state databases
- AI-enhanced workflows: Accelerate document classification, policy management, and credentialing tasks
- Managed credentialing: Access optional specialist teams for hands-on credentialing support
Pricing
Tiered pricing. Pay-for-what-you-need model.
Pros
- Only platform unifying credentialing, compliance, and learning in one product
- Named to G2's 2026 Best Software Products list; rated 4.4 stars across 86 reviews
- Support team answers 95% of calls within two rings
Cons
- Credentialing depth may not match purpose-built CVO platforms
- Strongest fit for organizations needing compliance training alongside credentialing
- Enterprise compliance features add complexity that pure telehealth startups may not require
7. Modio Health
Best for: Telehealth staffing agencies and distributed care organizations needing a central system of record for provider credentials
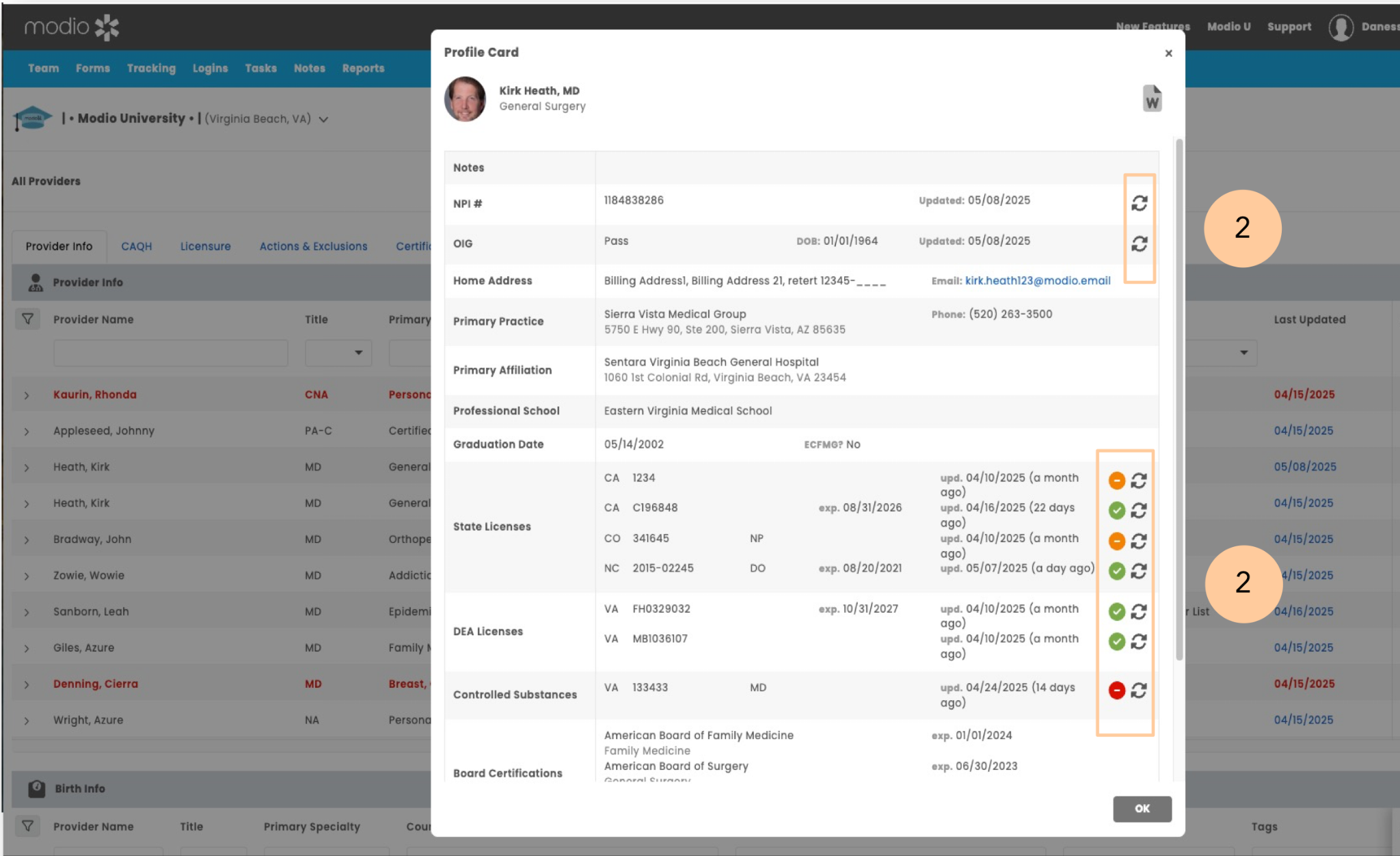
Modio Health is a provider credentialing management platform built around a concept they call OneView: a centralized credential profile for each provider that aggregates their licenses, certifications, and credentialing documents in one place.
It's used across health systems, group practices, and staffing companies, and it has been around long enough to be a known name in the credentialing space.
Key Features
- Centralized credential storage: Store provider documents with automated expiration alerts across distributed teams
- Self-serve provider portal: Let providers upload documents and update profiles independently
- Manual PSV: Access data from 100+ primary sources with on-demand verification triggers
- CAQH monitoring: Track profile status and re-attestation deadlines
Pricing
Custom pricing. No setup fee on entry-level tiers.
Pros
- Intuitive interface praised across review platforms
- Strong fit for staffing agencies managing high provider volumes across states
- SOC 2 Type II certified with single sign-on support
Cons
- Does not execute managed licensing
- Verifications require manual initiation, not continuous monitoring
- No API available for custom system integration
How to Choose the Right Credentialing Software for Your Telehealth Organization
First, how much of the work do you actually want to own?
Some tools give you software and leave the credentialing work entirely to your team. Others handle everything on your behalf. Most growing telehealth organizations land somewhere in between: maybe one person managing the platform while a vendor handles the actual file processing.
Make sure the model fits how your team is structured before you get into feature comparisons.
Second, what does turnaround time actually mean for your operation?
Two weeks sounds fine until you're onboarding providers every month, and each one sits idle for half of it. Ask vendors for their actual SLA, not a range, and ask whether they hit it consistently.
There's a difference between "our average is around two weeks" and a 48-hour SLA with a documented compliance rate.
Third, how does the tool handle CAQH?
If your team is logging into CAQH separately and copying data over by hand, that's not integration, that's just having two tabs open. Real CAQH integration means provider data flows in automatically and stays in sync.
Fourth, is the vendor NCQA-certified?
If you're operating under delegated credentialing arrangements, this matters a lot. It simplifies your audit process significantly and signals that the vendor's processes have been independently reviewed.
You also need to look at…
Multi-state PSV and licensing infrastructure
Telehealth providers practice across state lines, which means credentials need to be verified and monitored in every jurisdiction. Your vendor should run PSV in parallel rather than sequentially and manage license renewals across all active states without manual tracking.
IMLC and PSYPACT compact expertise
Interstate compacts reduce the number of state licenses a telehealth provider needs. Your vendor should evaluate eligibility on a provider-by-provider basis and manage compact applications alongside traditional licensing.
Continuous monitoring across jurisdictions
A credentialing file is only valid at the moment it's completed. For telehealth organizations with providers in dozens of states, continuous monitoring that flags sanctions, license expirations, and board actions in real time is essential.
Enrollment capabilities (separate from credentialing)
Many telehealth organizations need their credentialing partner to handle payer enrollment as well. If that applies to you, evaluate whether the platform supports virtual address validation, closed panel detection, telehealth-specific payer restrictions, and proactive follow-up on stalled applications.
Still Deciding? Here's How We'd Narrow It Down
Credentialing is one of those things that feels administrative until it starts slowing you down. For telehealth organizations, the multi-state complexity means it slows you down faster and more often than it does for traditional practices.
Most of the tools in this list handle the basics. The meaningful differences show up in how well they handle volume, how much automation they actually deliver on primary source verification, and whether they were designed with telehealth operations in mind.
We built Assured specifically for organizations like yours. We credential providers in 48 hours, integrate directly with CAQH, monitor credentials across 2,000+ sources, and bring real telehealth experience to every client we work with. If you want to see how it works in practice, we can have you live in under 72 hours.
Frequently Asked Questions
What is the difference between credentialing and payer enrollment?
Credentialing is the process of verifying a provider's qualifications: their education, licenses, board certifications, work history, and disciplinary record. Payer enrollment is a separate process that gets a provider accepted into an insurance network so they can bill for services. The two are often handled by the same vendor but are distinct workflows with different timelines and requirements.
How long does credentialing take for a telemedicine provider?
It depends on how many states the provider is licensed in and which verification steps are required. With manual processes, a single provider file can take weeks to compile. Automated platforms like Assured compress that to one to two hours. Full processing time from submission to completed file averages 48 hours with Assured, compared to an industry norm of around two weeks.
Do telemedicine providers need CAQH profiles?
Yes, and it's worth requiring it as a condition of onboarding. CAQH is the standard repository for provider credentialing information, and it eliminates significant manual data entry when your credentialing platform integrates with it directly. Most credentialing platforms support CAQH in some form, but the quality of that integration varies considerably.
What is NCQA certification and why does it matter for credentialing?
NCQA (National Committee for Quality Assurance) certification means a credentialing organization has been independently evaluated against defined quality standards. For telehealth organizations operating under delegated credentialing agreements with health plans, working with an NCQA-certified credentialing vendor simplifies the audit process considerably.
Can credentialing software handle providers licensed in multiple states?
Most platforms can track multi-state licenses, but the depth of support varies. You want to confirm that the platform monitors expirables across all active states, supports state-specific application requirements, and integrates directly with the primary sources in each state. For telehealth organizations with providers in 20 or 30 states, this is one of the most important things to verify before choosing a tool.
What are interstate licensure compacts?
Agreements between participating states that create expedited multi-state licensing pathways. The IMLC covers physicians, the NLC covers nurses, and the PSYPACT covers psychologists. They reduce licensing timelines but do not replace PSV. Learn more about network management.


.svg)
.png)



.svg)
.png)


